Phage Therapy

Phage Susceptibility Test
Phages may play a significant role in treating complex bacterial infections in prosthetic joints, according to new Mayo Clinic research. The findings suggest phage therapy could provide a potential treatment for managing such infections, including those involving antibiotic-resistant microbes.
Phages are naturally occurring viruses found throughout the earth that target and kill specific bacterial cells, including those that have grown resistant to multiple antibiotics. The microscopic organisms destroy bacteria by injecting their DNA or RNA into the bacteria to replicate and burst the cells open.
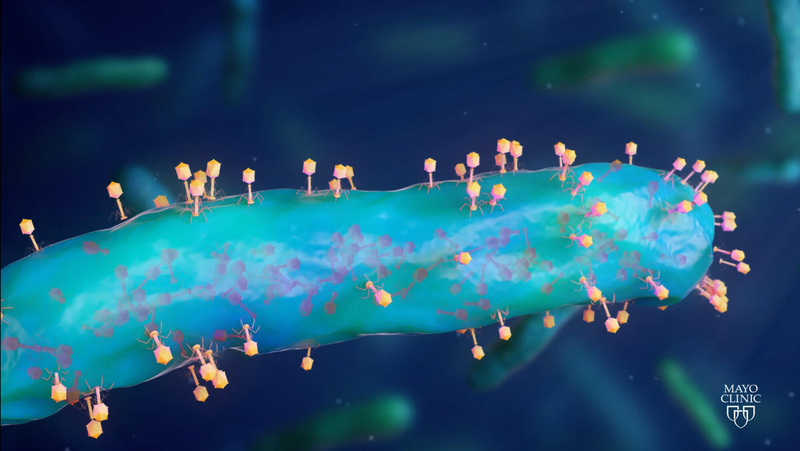

Biofilms and evading antibiotics
Mark Pearce, 61, was facing a possible limb amputation, even death, when a multidrug-resistant bacterial infection within his prosthetic hip replacement device started raging in his bloodstream. In the spring of 2020, with a fever at more than 105 degrees, Mark was taken to Mayo Clinic Hospital in Rochester. Mark had been battling the chronic bacterial infection on and off since 2014.
Bacterial infections are a known risk among the millions of people worldwide who undergo life-enhancing joint replacements every year. The issue is that bacteria can clump together and grow into a slimy protective coating, called biofilms. These biofilms cling to the implanted devices and enable bacteria to evade antibiotics that would otherwise work against them.
Despite multiple treatments and three additional hip replacement operations, Mark’s condition continued to worsen.
“Mark’s case was quite challenging, given the aggressive organism (MRSA), the failure to respond to multiple prior surgical interventions, and extensive allergies to antibiotics which limited our choice of antibiotics.” Gina Suh, M.D.
A potential alternative
That’s when his Mayo Clinic health care team turned to an experimental treatment approach — bacteriophage therapy. The strategy, also called phage therapy, uses viruses to target and kill specific bacteria.
“There is increasing evidence that phage therapy can serve as a potential alternative or supplement to antibiotics to eradicate recalcitrant bacterial infections,” says Gina Suh, M.D., director of Mayo Clinic’s Phage Therapy Program, which was launched by the Center for Individualized Medicine in 2019. Dr. Suh is Mark’s phage therapy physician.
Putting phages to use
Mark received his first phage therapy intravenously in the summer of 2020. His treatment continued five days a week for several weeks. This was followed by hip removal and replacement surgery performed by Mark Pagnano, M.D., Professor and Chairman with the Department of Orthopedic Surgery.
“I have cared for Mr. Pearce for more than 20 years, and he has been through more than his fair share of medical issues,” Dr. Pagnano says. “The availability of phage therapy opened up a unique opportunity to treat this very difficult infection in a different way here at Mayo Clinic.
Mark Pearce says he started feeling better almost immediately after receiving phage therapy. Mark was Mayo Clinic’s fourth patient to receive the investigational phage therapy treatment under a compassionate use basis.
Phages and the future
“As we continue to evaluate this novel therapeutic, we will continue to learn about the role phages will play in treating different infections,” Dr. Suh says. “In some infections, phages and antibiotics alone may do most of the work. However, I think in cases of chronic surgical infections like this, the surgery was the star of the show and phages played a supporting role. Nonetheless, both modalities together have resulted in a good outcome for Mark, and that is ultimately the goal.”
Dr. Suh is working to make phage therapy more broadly applicable. She is launching two clinical trials in 2022 to continue to evaluate phage therapy in the treatment of prosthetic joint infections and pressure injury wounds.
Share this story
A version of the story was originally published in Mayo Clinic’s News Network and Mayo Clinic’s Individualized Medicine blog.
Mayo Clinic and Dr. Suh each have financial interest in the technology referenced in this article. Mayo Clinic will use any revenue it receives to support its not-for-profit mission in patient care, education and research.
